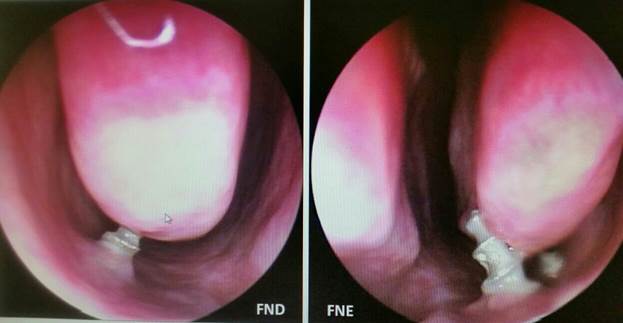
Fig. 1: Rough compression-screw implants inserted too deep into the nasal cavity, projecting several millimeters into the airway. Postoperative radiograph of the clinically inconspicuous situation 24 months after implantation. Since no masticatory forces are transmitted in the area of the airways anyway, this deep insertion of the implant makes no sense. While a constant flow of air and fluids in the nasal cavity helps prevent inflammation, much less favorable conditions are present in the maxillary sinus: if the same (rough-surface) implants are placed here, granulation and chronic inflammation will often occur, something that is not observed in association with the nasal cavity.
Internationale Implantatstiftung
Wir sind eine gemeinnützige und wissenschaftlich ausgerichtete Stiftung des Privatrechts, die Patientenerfahrungen und Ergebnisse von
Zahnimplantat-Versorgungen nach Knochenaufbau
erfassen und bewerten möchte.
Ziel ist die Erstellung einer Studie zur dentalen Versorgungsrealität in Deutschland / Österreich / Schweiz.
Einsender (Patienten u.a.) erhalten eine fachliche Einschätzung und Bewertung, kostenfrei und vertraulich.
Bitte wenden Sie sich an:
Internationale Implantatstiftung München
contact@implantfoundation.org
5th Consensus on Treatment Modalities with Basal Dental Implants in Connection with the Maxillary Sinus
(Version 3, released with illustrations in May 2018)
Other applicable IF consensus documents:
- Consensus on basal implants:
www.implantfoundation.org/en/consensus-on-basal-implants-2018 - Exploratory consensus:
www.implantfoundation.org/de/sondierungskonsensus2016
1. Clinical anatomical description of the maxillary sinus
The human body consists of bones, soft tissue, and fluids. Voids (that is, spaces inside the body that are not filled with any of these components) exist in the oral cavity, the nose and sinuses, and in the airways. Nevertheless, the body may fill even these cavities with soft tissue and/or fluids so that a medical intervention may become necessary to remove or reduce these substances or structures.
Technically, the maxillary sinus constitutes a blind hole to that has only a single natural opening, namely to the middle nasal passage (meatus nasi medius). The healthy maxillary sinus is capable of self-cleaning through this natural opening. If the opening (suddenly) becomes too for the amount of secretion to be removed, or if it is blocked, this will lead to a backlog of fluid in the sinus. Soft-tissue neoplasms in the maxillary sinus (mucoceles, granulation tissue) can relocate the natural drainage path and achieve enough vascularization to survive permanently in the maxillary sinus. This is true of benign and malignant tissue formation alike. More than 90% of all such clinical problems or tissue neoplasms originate in the medial maxillary sinus wall or the orbital floor. The posterior maxillary sinus (the areas of the molars) can hardly be the origin of drainage obstruction because these areas are too far away from the site of the natural outflow from the maxillary sinus.
From a developmental point of view, the maxillary sinus is an air-filled cavity that is almost completely surrounded by bone, lined with a membrane. It is simply a relic of the atrophy of the surrounding bone, which will be manifest to different extents and continue throughout life. Unfortunately, the size of the ostium is not determined by any actual clinical need but by functional parameters related to the bone (atrophy, remodeling, reactive bone formation, etc.). The position and extent of the nasal concha, which may additionally or by themselves restrict the function of the ostium, are not influenced or controlled by the clinical need for drainage. These latter circumstances alone often require surgical intervention in order to facilitate an adequate discharge from the maxillary sinus.
The maxillary sinus tends to increase in size throughout life. This process of atrophy is subject to Wolff’s law, according to which the bone optimizes its shape and volume (i.e., bone mass will decrease as a result of sufficient maintenance) and adapts to the function it serves.
In the healthy state, the maxillary sinus is equipped with a thin membrane and cilia. It cleanses itself by secretion (about 1 liter per day) and adequate secretion removal and is almost always free from microorganisms.
Pathological developments (or transient rhinogenic inflammation) in any region of the maxillary sinus can increase the secretion or cause the formation of new tissue, which often leads to the drainage path through the natural ostium being overloaded or the natural ostium being blocked.
The Schneiderian membrane is the inner lining of the maxillary sinus; it has its own intra-sinus blood supply. In its healthy state it is very thin – particularly thin in smokers, but can increase in thickness in nonsmokers. If the membrane thickens or if inflammation (such as a dental infection) has to be combated continuously, there is an additional need for an inflow and outflow of blood. This results in chronic inflammatory conditions. If new tissue formation is caused by foreign bodies displaced into the maxillary sinus, no (self-) healing can be expected as long as these foreign bodies are not removed. In this respect, these very foreign bodies require accessing the maxillary sinus surgically (modified Caldwell-Luc fenestration procedure).
In situations where self-cleaning of the maxillary sinus is limited in the presence of granulation, cysts, or mucoceles, the insertion of a basal implant, which naturally extends into the maxillary sinus or is even placed through the sinus, can “tip the balance.” While this situation is unpredictable, it must and can be adequately addressed. There is hardly any danger to the implant per se if the (natural) ventilation or some other form of drainage is restored quickly to the maxillary sinus.
Conventional medical training at universities in many Western countries (ENT, dentistry) and the rules laid down by the national health insurance systems call for most, even recurrent, problems of the maxillary sinus to be treated conservatively with nasal rinses, decongestant nasal drops, and antibiotics; these will in fact often bring about improvement in the medium term. However, in many cases this type of treatment does not address the root cause of the problem. This is why recurrences are regularly seen, e.g. in the fall season or allergens are present at higher concentrations in the vicinity of the affected patient. The (unnecessary) treatment of the recurrences cause unnecessary pain and outbreaks in affected patients and will also drive up the cost to the respective health insurer considerably. The only long-lasting successful therapy of chronic drainage obstructions is the creation and maintenance of efficient and permanently adequate ventilation and adequate drainage from the maxillary sinus.
The first pertinent surgical procedure described was the Caldwell-Luc procedure (performed under general anesthesia) in which the antrum wall between the teeth and the infraorbital foramen was opened, allowing the contents of the sinus to be removed completely and with ease. A drawback of this procedure, as previously stated, was the not uncommon scar-related tension exerted on the infraorbital nerve and the associated chronic pain. This drawback has led to conservative treatments being in continued use. Later, a procedure was developed in which the reconstruction of the maxillary sinus with a titanium mesh (for example) achieved a predictable separation of the maxillary sinus and facial soft tissue. This can minimize or even prevent the pain caused by scarring.
Only with the introduction of endoscopic procedures (which are performed under sedation or anesthesia) was a reliable and almost side effect-free surgical method developed to surgically ensure adequate sinus drainage.
2. Treatment options in the region of the maxillary sinus
The placement of dental implants in the area previously occupied by the maxillary sinus are now a dental standard and an established adjunct in conventional medicine.
There are two fundamentally different modalities of implant placement:
a. Implant treatment with bone augmentation and subsequent osseointegration
b. Cortical anchoring of dental implants without bone augmentation, via osseofixation
2.a. Bone-building therapy in the maxillary sinus area
If the vertical bone height between the crestal cortical bone of the distal maxilla and the basal cortical bone of the maxillary sinus is reduced, two treatment strategies are available to increase the bone supply in traditional implantology:
Open “sinus lift” procedures involve opening the vestibular wall of the maxillary sinus, lifting the Schneiderian membrane, and inserting bone replacement material between the Schneiderian membrane and the basal bony bed of the alveolar process. Internal sinus lifts are performed from caudally, sometimes without flap formation.
These procedures can sometimes be performed simultaneously with the placement of dental implants, otherwise separately. If the procedure is performed without simultaneous implant insertion, the waiting time between the “sinus lift” and the insertion of a conventional implant will be between three and five months. Typically, two-phase implants are used after sinus-lift surgery. These are large-diameter cartridge-shaped implants with rough endosseous surfaces.
As an alternative to the “sinus lift” with a bone substitute, bone blocks (bone grafts) can also be inserted. It should be borne in mind that this type of treatment is more invasive, as a bone block must first be removed elsewhere, which is associated with added risks and increased morbidity at the harvesting site. A more advanced variant of this method today forms the simultaneous insertion of two-phase implants in the bone block. However, immediate loading is not possible with this variant under normal circumstances, since immediate loading by necessity requires direct contact of the implant or abutment with the oral cavity; as the bone graft is sensitive to infection, immediate loading is usually avoided.
Thanks to the development of basal or basal/strategic implantology from about 2006, bone block surgery and sinus lifts performed to create more bone for anchoring dental implants in essence became superfluous. Nevertheless, they are still performed today — and in some places even frequently.
2.b. Cortical anchoring of dental implants without bone augmentation, via osseofixation
The use of lateral basal implants has evolved over the past 25 years as an alternative to conventional dental implantology, allowing immediate loading and avoiding bone augmentation. The pertinent treatment protocol requires only cortical anchoring of the implants in the cortical bone (“2nd cortical,” “3rd cortical”), one of which may be the basal bone bed of the maxillary sinus. To resist both intrusive and extrusive forces, the cutting threads of the implants must be screwed directly into the cortical floor of the maxillary sinus. The mere contact of the implant tip with the sinus floor is not sufficient for the function of the implants, because extrusive forces (which mainly occur with circular restorations) cannot be absorbed.
Basal implants have a thin and polished shaft1 and apical retentions (cutting threads or rings/disks). The implants are osseofixated either vertically or transcortically/horizontally. “Osseofixation” in this context means that the cutting threads of the implants engage the basal cortical bone of the maxillary sinus, so that the implant tip automatically comes to rest in the maxillary sinus, or at least in the thickened Schneiderian membrane.
The principles of osseofixation are well known from traumatology and orthopedic surgery. In the maxillary sinus region, osseofixation avoids the granulations known from two-phase implants with a rough endosseous surface; the intra-sinus parts of the polished basal implants do not retain infectious agents.
Since the cortical floor of the maxillary sinus is not one of the 100% safe implantation sites, implant designs usually provide for additional anchorage in e.g. the nasal floor or in the tuberopterygoid region.
Anchorage in the area of the zygomatic bone can be considered an alternative to anchorage in the floor of the maxillary sinus.
The situation after inserting basal implants into the sinus floor differs significantly from the situation after inserting conventional two-phase implants with a rough endosseous surface. Deep insertion (more than about 2 mm) of conventional dental implants with conventional rough surfaces in the maxillary sinus will in many cases lead to localized polyposis. In these cases, the implant tips behave like other foreign bodies (such as residual restorative materials or residual root fragments) in the maxillary sinus, provoking the formation of granulation tissue that takes up space. This form of polyposis can remain unnoticed and clinically inconspicuous for a long time.
Due to the considerable failure rate of “sinus lift” operations, a clear shift towards alternative, less risky methods is seen today. Another reason for the increasing rejection of sinus-lift procedures by patients is the fact that it makes immediate impossible. Patients no longer accept (unnecessary) bone augmentation day. They are also generally unwilling to accept prolonged “healing”/treatment times, added risk, collateral damage, and higher cost.
3. Maxillary sinus: morbidity and treatment
The prevalence of maxillary sinus problems in the population is significant, but in many cases its symptoms, associated with nasal inflammation, later disappear again. If symptoms of the maxillary sinus persist and adversely affect the patients’ quality of life, surgical correction of the anatomy of the maxillary sinus is the treatment of choice. Although open sinus correction (modified Caldwell-Luc surgery) is still performed today, minimally invasive techniques are spreading. The latter are successfully used in cases where no iatrogenically inoculated foreign bodies in the maxillary sinus have to be removed under visual control. If Corticobasal® implants are firmly anchored in the second cortex, with or without penetration of the Schneiderian membrane, they are not considered foreign bodies. They are not removed in the case of maxillary sinus infections, as they are presumably not involved nor the cause of the problem. With their smooth surface, they do not maintain any inflammation.
Fig. 2: Granulations, polyps and other unwanted tissues will not shrink nor disappear unless the cause of the granulation has been removed.
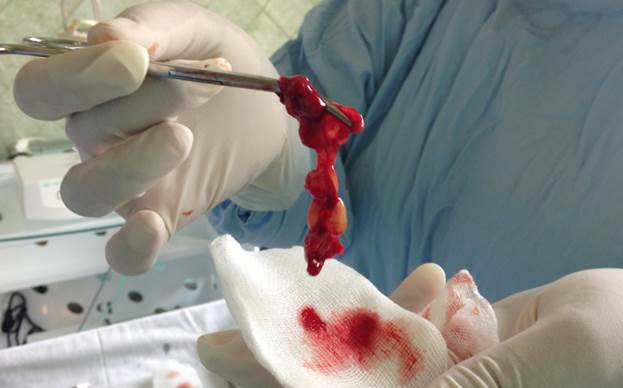
If a radical procedure is performed, the treatment objective will be to completely remove the cause of the problem or problems. For this reason, all affected soft tissue (granulation, polyposis), relics of dental therapy, residual root fragments, implant components, etc. are completely removed using a lateral approach (Caldwell-Luc), providing, in addition, sufficient ventilation through the natural ostium. Facilitating unimpeded ventilation is another objective of this procedure. Lateral basal implants can be inserted directly at the same time. The (surgically created) bony opening in the vestibular sinus wall can be closed, for example, with a titanium mesh. This treatment uses an antibiotic (such as moxifloxacin hydrochloride) as well as a local disinfectant (such as povidone-iodine) and tamponades.
The objective of endoscopic treatment via the nasal route is to expand the natural ostium and to remove the uncinate process, providing optimal ventilation and, in a high percentage of cases, subsequent self-healing.
Alternatively, especially for the immediate treatment of acute disease processes, an additional opening in the lower nasal cavity — towards the maxillary sinus — can be created. Such additional openings later often close by themselves. There have been reports that these openings can cause circulation between both ostias without providing ventilation to the rest of the maxillary sinus, which should be considered an unfavorable variant.
It can be very helpful to flush the maxillary sinus with local disinfectants. If these treatment attempts do not provide a significant improvement within a few days, surgical therapy should be considered.
Antibiotics must be sufficiently highly dosed and effective to truly improve the situation of the inflamed maxillary sinus rather than contributing to an undesirable chronification.
4. What precautions are necessary if the treatment plan for a dental implant provides for the insertion of cortical implants in the basal or palatal/lateral cortical bone of the maxillary sinus?
There are many different health impairments potentially caused by infections of the maxillary sinus.
A significant percentage of the population shows clinical signs of recurrent infection of the maxillary sinus (e.g. always in fall/winter and in spring due to particularly severe immune reactions to specific allergens). Treatment usually consists of prescribing antibiotics and locally applied ointments or rinses through the nose (including sodium chloride) to prevent or treat swelling. Most patients will oppose surgical correction as long as their quality of life does not suffer significantly from recurrent or permanent infection. These patients trivialize the problem at the symptom-free stage, and many of them do even report these passing afflictions with their medical history — even when explicitly requested to do so.
During a temporary deterioration of the condition, the Schneiderian membrane appears thickened. Either on its own or in combination with cysts, mucoceles, or other soft-tissue contents of the maxillary sinus, the membrane can displace the natural ostium and thus block the drainage.
The total thickness of the Schneiderian membrane is usually well below 12 mm; in smokers, this membrane is very thin. The presence of a thicker membrane suggests polyposis. Swelling of the intra-sinus soft tissue can block the natural ostium and stimulate pus formation in the maxillary sinus.
Pus and other secretions will always seek the path of least resistance to leave the maxillary sinus. Once the natural drainage pathway has been blocked, recurrent fistulas may form or the secretions may drain via the fresh implant site.
A full 90% of all clinical problems in the maxillary sinus originate in the medial sinus wall, the medial orbital floor, or the basal sinus wall. Changes or events in the distal or distolateral area of the maxillary sinus almost never affect the drainage status. This is one of the reasons why clinically manifest problems related to the insertion of so-called zygomatic implants (even trans-sinus ones) rarely occur
It is important to avoid inserting two-phase implants into the maxillary sinus (except in the context of a Summers sinus lift or an open sinus lift) during the acute phase of an inflammation. However, acute phases cannot be diagnosed while there are no clinical symptoms (fever, pain, feeling of pressure, discharge of pus).
Particulate residue from dental treatments (restorative materials, root-canal filling material, root fragments, even endodontic instruments or parts thereof) are often found inside maxillary sinuses. They are then permanently encapsulated by granulation tissue. Without a (radical) surgical intervention and removal of the objects, no regression of the Schneiderian membrane or healing of the polyposis or granulation can be expected.
5. Are there any absolute contraindications to the insertion of basal implants in connection with the maxillary sinus?
Experience has shown that surgical restoration of the maxillary sinus (e.g. Caldwell-Luc or an endoscopic extension of the natural ostium) is a safe therapy and that these interventions can also be carried out later on an as-needed basis (i.e. after implant placement, as problems occur). As a result, basal screw implants or combination designs can be used even in less favorable situations. However, it should be noted that no rough surfaces should be inserted into the maxillary sinus transcortically, as this can lead to retrograde peri-implantitis and the retention of bacteria on the rough implant surface.
Patients should be informed that the treatment approach using traditional basal screw implants and combination designs deviates from the earlier approach for two-phase implants for good reasons and that not all (future) treatment providers will be sufficiently cognizant of the special features mentioned above.
It is well known that many patients prefer to live with recurrent or even chronic infections of the maxillary sinus and shy away from surgery. Potential problems related to the insertion of basal screw implants inside the maxillary sinus must be considered separately; they usually have nothing to do with the implants. Granulation, polyposis, soft-tissue changes, and suppurations can generally be treated successfully without removing the implants. It is therefore considered unethical to deny this group of patients the treatment with basal implants merely because they refuse to undergo preimplantological procedures in or on the maxillary sinus.
6. Is mobility of basal dental implants an indication for implant removal if the implant is connected to the maxillary sinus?
6.a.
Mobility in conventional crestal implants with rough endosseous surfaces and large diameters is a clear indication for their removal because the implant surface can promote the migration of intraoral bacteria into the maxillary sinus, and re-osseointegration of the implant after the general inflammation in the maxillary sinus has subsided is unlikely. But implants of thus type are not indicated for use within the maxillary sinus at any rate.
The formation of bony craters around the tip of the crestal implant (i.e., signs of retrograde peri-implantitis as diagnosed by CT scans or other radiographic methods) usually requires the implant to be removed. At an advanced stage, the resorptive fronts of orthograde and retrograde peri-implantitis will meet, and the affected implant becomes mobile and fails.
6.b.
Cortically anchored jaw implants are routinely inserted into the lower/basal cortex of the maxillary sinus (or through the sinus). The final position of the implant tips — and not infrequently also a part of the thread — is within the maxillary sinus. The same result in terms of the final position is achieved after orthopedic surgery or midfacial trauma surgery.
The “Consensus on basal implants” (1999, 2006, 2015, 2018) can be consulted to determine whether and when basal implants must be removed. Lateral mobility or the possibility of rotation are no mandatory indications for the removal of basal implants. Vertical mobility, by contrast, indicates that removal of the implant is likely to be necessary. A correct clinical diagnosis — and thus a decision for or against implant removal — is facilitated if no splinting prosthetic elements are attached to the implant and if each implant can be assessed on its own merits.
Implantologists trained in the use of basal implants receive appropriate specialist training during their product-specific postgraduate continuing education. For this reason, decisions regarding critical treatment phases should be entrusted to these implantologists only. Nevertheless, it will often be advisable to discuss the extent of ay remedial therapy of the maxillary sinus in individual cases in cooperation with ENT specialists.
7. Method of direct insertion of lateral basal implants in patients with purulent inflammations of the maxillary sinus
Patients with recurrent or chronic inflammation of the maxillary sinus should be informed that it is advisable to treat their disease prior to implant placement. However, it is difficult to determine whether such treatment was carried out correctly or at all and whether it will be successful in the medium or long term.
The insertion of large and rough two-phase implants into the maxillary sinus (including penetration of the Schneiderian membrane and without performing a sinus lift) is contraindicated in existing or known recurrent or chronic inflammations of the maxillary sinus.
Conservative approach
A more conservative approach, that is, implantation even in the presence of demonstrated or suspected inflammation within the maxillary sinus, is possible if basal screw implants are used.
The process involves transcortical osseofixation and the use of a local disinfectant (such as povidone-iodine). Since problems within the maxillary sinus are not the target of this therapy and are therefore left unattended (except for minimal doses of 5% povidone-iodine in the affected sinus), recurrent or chronic maxillary sinusitis will often persist.
If possible, it should be ensured that the implants inserted do not transfer the inflammation into the area of the 2nd or 3rd cortical.
If the natural drainage paths are nearly closed, implantation in the maxillary sinus area can lead to the compromised drainage capacity suddenly being exceeded, resulting in an exacerbation of the inflammation.
Since lateral basal implants exhibit a dual healing mode, infections within the maxillary sinus are more likely capable of preventing their healing (osseointegration after filling the slot areas with woven bone). Basal screw implants do not exhibit this shortcoming or only to a much lesser extent.
If the condition should worsen at a later stage (after the integration of the implants), the patient should again be advised of the surgical treatment option. In this case, the treatment of choice will be either
- an endoscopically controlled enlargement of the natural ostium or
- the creation of an additional opening from the lower nasal cavity to the maxillary sinus,
whereas in cases where foreign bodies are embedded in granulation tissue (especially at a distance from the maxillary sinus floor), radical measures (modified Caldwell-Luc surgery) should probably be resorted to.
In endoscopic treatments to widen the connection between the maxillary sinus and the nose, dental therapy residues are often not removed, yet these approaches produce adequate ventilation in the vast majority of cases and infection removal in around 95%, as well as recovery within a few days or weeks. All this without any further treatment requirement.
Basal implants are not clinically affected by intra-sinus procedures, which only address the intra-sinus soft tissue only. Integrated or rigidly osseofixed polished implants are not considered to be the cause of the problem unless other findings (such as retrograde peri-implantitis on CT scans or x-rays or vertical mobility of the implants) indicate an involvement.
If the conservative approach is chosen, patients must be informed in detail about the possible need for additional treatment of the maxillary sinus and about the fact that ENT specialists may not be familiar with the different treatment modalities of dental implants or the special features of basal implant therapy. Qualified advice and help from dentists can only be expected if they have received special training related to the handling of cortically anchored implants.
8. Consequences of slow natural expansion (pneumatization) or a possible increase in bone mass in the maxillary sinus
In the lower maxillary sinus, this expansion process is usually described as “sinus expansion” or “ventilation,” which does not adequately describe the real cause of the process. Any surgical procedure in this area triggers a further boost in bone modeling and remodeling, causing the maxillary sinus to expand and more bone of the maxillary alveolar process to be lost. Therefore, additional atrophy is to be expected after implantation, which may ultimately even lead to the basal edge of the maxillary sinus expanding so much that the previously inserted transcortical threads of the basal screw implants lose all contact with the basal cortical bone of the maxillary sinus. Once this is the case, these implants no longer play a role in the transmission of force. They can be removed or screwed back into the cortical bone counterclockwise (if the prosthetic superstructure allows this).
Previously osseointegrated lateral basal implants (which were not attached to the outside of the maxillary sinus or the zygomatico-alveolar crest with additional screws) may also lose contact with the cortical bone due to the expansion of the maxillary sinus (especially in the region of the first and second premolars and the first molars) and thus become mobile.
Figs. Y a and b: However, the exact opposite development is also observed: if basal/strategic implants are inserted into the base of the maxillary sinus, bone augmentation may occur in the implantation area. There are two reasons for this:
a. If bleeding into the maxillary sinus occurs during implantation, the blood clot can stabilize in the sinus and lead to the formation of woven bone. Next, new cortical bone forms further inside the sinus and the cortical bone initially used for anchorage is resorbed — the implant loosens.
b. b. Likewise, the occlusal force transferred to the bone via the implant can lead to an increase in the bone mass and to improved bone quality. But bone augmentation can also cause the implant to lose contact with the cortical bone.
9. Surgical technique and the use of systemic antibiotics and local disinfectants
Once the access channel for the insertion of cortically anchored implants has been drilled, care should be taken to prevent loose bone particles from penetrating into the maxillary sinus. It may be useful to flush the intrabony canal with 5% povidone-iodine prior to implant placement. Bone particles introduced into the maxillary sinus by this route can promote infection if the preoperative borderline condition of the maxillary sinus already prevented self-healing.
The use of systemic (oral) antibiotics as a prophylactic measure in implant treatment has not been demonstrated to be a (safe) way to promote implant success or to prevent inflammation within the maxillary sinus.
In traumatology and in orthopedic surgery, local disinfectants (such povidone-iodine) are routinely used to prevent local infection. This approach is also recommended when placing basal jaw implants — in all areas of the jaw.
10. Summary
The need for restorative surgery within the maxillary sinus depends directly on the condition of the maxillary sinus itself or the remnants of dental therapy inside this anatomical structure.
The insertion of basal screw implants with supported by the cortical bone of the maxillary sinus (osseofixation) is currently the most modern method of treatment, even if one or more of the following pathologies are present inside the sinus:
- Thickening of the Schneiderian membrane
- Polyposis
- Mucoceles
- Remnants of fillings or residual root-filling material
Before lateral basal implants can be placed through the sinus, the maxillary sinus must be clinically free of infection and no remnants of dental treatments or other objects must be present in the sinus, because the successful dual healing mode of these implants requires the formation of callus. The ventilation of the antrum must be checked intraoperatively, for example with the nasal blow test. Granulation tissue, polyps, mucoceles, cysts, and dental implant residues are removed the Caldwell-Luc procedure, often in conjunction with the insertion of the implant or implants. This radical approach to therapy represents the current state of the art. Since a flap must be reflected for lateral basal implants in any case and since the insertion of the implants can optionally be performed through the sinus, the minimal extension of the scope of the procedure to include a Caldwell-Luc is not associated with a significant increase in invasiveness. This procedure is considerably less invasive than bone block grafts, as these are associated with considerable additional risks and morbidity at the donor sites.
The insertion of conventional two-phase dental implants in which the rough endosseous surface penetrates the Schneiderian membrane is contraindicated. It would typically lead to recurrent chronic or acute infections of the maxillary sinus as well as retrograde peri-implantitis.
Basal screw implants with machined/polished surfaces, on the other hand, can be screwed into the maxillary sinus or inserted through it (e.g., when anchored in the zygomatic bone) according to the state of the art. The cutting threads of these implants must be anchored in the second or third cortical in such a way that stability on the presence of masticatory tensile and compressive forces is achieved. With cortico-basal anchoring in the maxillary sinus floor, this automatically causes apical thread portions to be located within the maxillary sinus. The procedure corresponds to that traditionally carried out in traumatology and orthopedic surgery (especially when the maxillary sinus was involved).
The cortical floor of the maxillary sinus represents a region of reduced stability of the (second) cortical. A sufficient number of mutually stabilizing implants must be placed; additional implants added in safer region of cortical bone (such as in the nasal floor or in the tuberopterygoid region) must also be included in the design.
References
Konstantinović V (2003): Aspekte der implantologischen Versorgung mit BOI im Bereich des Sinus maxillaris. ZMK. 19:568–575.
Richtsmeier WJ (2011). Top 10 Reasons for endoscopic maxillary sinus surgery failure. Laryngoscope. 2001 Nov. 111: 1952-6; PMID 11801976.
Besch KJ (1999): Konsensus zu BOI; Schweiz Monatsschr Zahnm. 109:971–972
1 The shanks of the Strategic Implant® can have a much thinner design because it is a one-piece implant where a detachable internal connection between the abutment and the endosseous implant body is not required. Furthermore, endosseous surface enlargement is not necessary because the primary permanent osseofixation stabilizes the implant sufficiently.




